Endocrine System
Introduction to the Endocrine System
The endocrine system is a crucial communication network within the body, working in conjunction with the nervous system to maintain homeostasis and regulate various physiological processes. Unlike the nervous system, which primarily uses electrical signals for rapid, short-duration responses, the endocrine system employs chemical messengers called hormones that travel through the bloodstream, eliciting slower, more sustained responses.
Overall Functions of the Endocrine System
The endocrine system is responsible for a wide array of vital functions, ensuring the body's proper growth, development, and adaptation. Its key roles include:
- Regulating Nutrient Metabolism and Water & Electrolyte Balance:
- This is fundamental for maintaining a constant internal environment (homeostasis). Hormones control how the body processes carbohydrates, fats, and proteins for energy, storage, or conversion. They also play a critical role in balancing water and crucial ions like sodium, potassium, and calcium, essential for cell function and overall fluid balance.
- Inducing Adaptive Changes to Help the Body Cope with Stressful Situations:
- The endocrine system orchestrates the body's "fight or flight" response and longer-term stress adaptation. Hormones like cortisol and adrenaline prepare the body for perceived threats by mobilizing energy stores and altering physiological functions.
- Promoting Smooth, Sequential Growth and Development:
- From fetal development through childhood and adolescence, hormones meticulously control the growth of tissues, organs, and the entire body. They also dictate the timing and progression of puberty and the maturation of reproductive organs.
- Controlling Reproduction:
- Hormones are central to all aspects of reproduction, including the development of sex characteristics, the regulation of menstrual cycles in females, sperm production in males, pregnancy, childbirth, and lactation.
- Regulating Red Blood Cell Production:
- Erythropoietin, a hormone primarily produced by the kidneys, stimulates the bone marrow to produce red blood cells, which are vital for oxygen transport.
- Controlling and Integrating Activities of the Circulatory and Digestive Systems (along with the Autonomic Nervous System):
- Hormones influence heart rate, blood pressure, blood vessel tone, and blood volume (circulatory system). In the digestive system, they regulate appetite, enzyme secretion, motility, and nutrient absorption. This integration ensures that these systems function efficiently and are coordinated with the body's overall needs.
Definitions
- Hormone: A hormone is a chemical messenger synthesized by specialized cells, typically within endocrine glands. These messengers are transported by the blood to target organs or tissues (their "site of action"), where they bind to specific receptors and cause an alteration in the function of the cell. An example is Growth Hormone, which promotes overall body growth.
- Endocrine Glands: Endocrine glands are specialized organs or tissues that synthesize and release classical hormones directly into the blood. They are often referred to as ductless glands because, unlike exocrine glands (which release secretions through ducts), their hormones are secreted directly into the bloodstream without the need for ducts. Examples include the thyroid gland, adrenal glands, pituitary gland, and pancreas (for its endocrine function).
Tropic Hormones
- Definition: Tropic hormones are a special class of hormones that have as their primary function the regulation of hormone secretion by another endocrine gland. The term "tropic" means "nourishing," which reflects their role in stimulating and maintaining their endocrine target tissues.
- Function: Tropic hormones not only stimulate the target gland to produce and secrete its own hormones but also maintain the structural integrity (trophic effect) of that gland. Without their tropic hormone, target glands can atrophy (shrink) and become underactive.
- Example: Thyroid-Stimulating Hormone (TSH): TSH is a tropic hormone secreted by the anterior pituitary gland. It stimulates the thyroid gland to secrete thyroid hormones (T3 and T4). Additionally, TSH maintains the normal size and health of the thyroid gland. In the absence of TSH, the thyroid gland would atrophy (shrink) and produce very low levels of its hormones, leading to hypothyroidism.
Complexity of Endocrine Function
The endocrine system, while seemingly straightforward in its definition, exhibits remarkable complexity in its operations:
- A Single Endocrine Gland May Produce Multiple Hormones: Many glands are multi-functional. For instance, the anterior pituitary gland is a master gland that secretes at least six different hormones, each with distinct target tissues and functions (e.g., TSH, Growth Hormone, ACTH, FSH, LH, Prolactin).
- A Single Hormone May Be Secreted by More Than One Endocrine Gland: Some hormones are produced by different endocrine sources, sometimes serving different roles depending on their origin. For example, somatostatin is secreted by both the hypothalamus (where it inhibits Growth Hormone release) and the pancreas (where it acts as a paracrine to inhibit insulin and glucagon secretion). In the stomach, somatostatin also acts as a paracrine to inhibit gastric acid secretion.
- A Single Hormone May Have More Than One Type of Target Cell and Induce Multiple Effects: Hormones often exert diverse effects by binding to different subtypes of receptors on various target cells.
- Example: Vasopressin (Antidiuretic Hormone - ADH):
- Water Reabsorption: Vasopressin promotes water reabsorption by the kidney tubules by binding with V2 receptors on the distal and collecting tubular cells. This helps conserve body water.
- Vasoconstriction: It also causes vasoconstriction of arterioles throughout the body by binding with V1 receptors on arteriolar smooth muscle. This helps increase blood pressure.
- Example: Vasopressin (Antidiuretic Hormone - ADH):
- Hormones with Multiple Target-Cell Types Can Coordinate Activities Toward a Common End: Sometimes, a single hormone's actions on different tissues converge to achieve a unified physiological goal.
- Example: Insulin: After a meal, insulin acts on muscle cells, liver cells, and fat cells. In muscle and fat, it promotes glucose uptake and storage. In the liver, it promotes glucose conversion to glycogen and fat synthesis. All these actions work in concert to store nutrients after absorption of a meal, thus lowering blood glucose.
- The Rate of Secretion of Some Hormones Varies Considerably in a Cyclic Pattern (Temporal Coordination): Endocrine systems often provide temporal (time) coordination of function, with hormone levels fluctuating in predictable cycles. This is particularly evident in:
- Reproductive cycles: Such as the menstrual cycle, where highly specific patterns of hormone secretion (e.g., estrogens, progesterone, LH, FSH) are required for normal ovarian and uterine function.
- Circadian rhythms: Many hormones follow a 24-hour cycle (e.g., cortisol, melatonin).
- A Single Target Cell May Be Influenced by More Than One Hormone: Target cells often possess receptors for multiple hormones, allowing for complex regulation and fine-tuning of their responses.
- Example: Liver Cells:
- Insulin: Promotes the conversion of glucose into glycogen within liver cells by stimulating specific hepatic enzymes.
- Glucagon: By activating different hepatic enzymes, glucagon enhances the degradation of glycogen back into glucose within liver cells. This antagonistic interaction allows precise control of blood glucose levels.
- Example: Liver Cells:
- The Same Chemical Messenger May Be Either a Hormone or a Neurotransmitter: The distinction between chemical messengers can sometimes be blurred, depending on their source and mode of delivery.
- Example: Norepinephrine:
- Hormone: Secreted by the adrenal medulla (an endocrine gland) into the bloodstream, acting on distant target cells.
- Neurotransmitter: Released by sympathetic postganglionic nerve fibers directly onto target cells at a synapse.
- Example: Norepinephrine:
- Some Organs are Solely Endocrine in Function, While Others Perform Non-Endocrine Functions as Well:
- Solely Endocrine: Organs like the anterior pituitary specialize exclusively in hormone secretion.
- Mixed Function: Other organs have both endocrine and non-endocrine roles. For example, the testes produce sperm (non-endocrine, reproductive function) and also secrete the male sex hormone testosterone (endocrine function). Similarly, the pancreas has both exocrine (digestive enzyme secretion) and endocrine (insulin, glucagon secretion) functions.
Glands and Hormones
I. Central Endocrine Glands
These glands, primarily located in the brain, serve as crucial regulators, often controlling the activity of other endocrine glands throughout the body.
A. Hypothalamus
The hypothalamus is a neuroendocrine organ, acting as the interface between the nervous and endocrine systems. It produces a variety of releasing and inhibiting hormones that primarily regulate the anterior pituitary gland.
- Hormones:
- Releasing Hormones:
- Thyrotropin-Releasing Hormone (TRH): Stimulates the release of TSH and prolactin from the anterior pituitary.
- Corticotropin-Releasing Hormone (CRH): Stimulates the release of ACTH from the anterior pituitary.
- Gonadotropin-Releasing Hormone (GnRH): Stimulates the release of FSH and LH from the anterior pituitary.
- Growth Hormone-Releasing Hormone (GHRH): Stimulates the release of GH from the anterior pituitary.
- Prolactin-Releasing Hormone (PRH): Stimulates the release of prolactin from the anterior pituitary (its existence as a distinct peptide is debated; TRH can also stimulate prolactin).
- Inhibiting Hormones:
- Somatostatin (Growth Hormone-Inhibiting Hormone, GHIH): Inhibits the release of GH and TSH from the anterior pituitary.
- Dopamine (Prolactin-Inhibiting Hormone, PIH): Inhibits the release of prolactin from the anterior pituitary.
- Releasing Hormones:
- Target Cells: Primarily the anterior pituitary gland.
- Major Functions: Control Release of Anterior Pituitary Hormones: The hypothalamus integrates neural input and secretes specific releasing or inhibiting hormones into the hypophyseal portal system, which then travel to the anterior pituitary, either stimulating or inhibiting the secretion of its own hormones. This forms the basis of many endocrine axes (e.g., HPA axis, HPT axis, HPG axis).
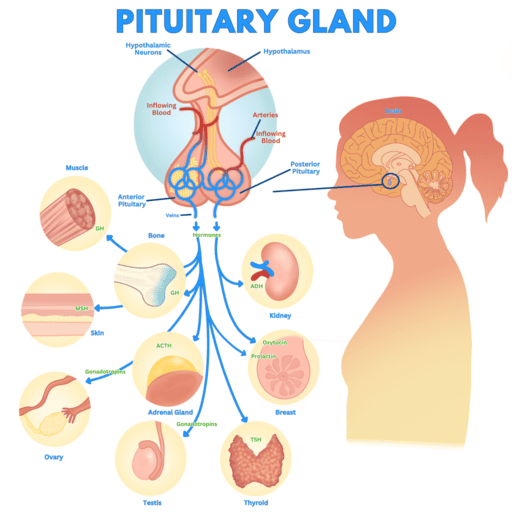
B. Posterior Pituitary (Neurohypophysis)
The posterior pituitary does not synthesize hormones; it stores and releases two hormones produced by neurosecretory cells in the hypothalamus (specifically the supraoptic and paraventricular nuclei). These hormones are transported down axons to the posterior pituitary for storage and release.
1. Vasopressin (Antidiuretic Hormone, ADH)
- Synthesis Site: Primarily supraoptic nucleus of the hypothalamus.
- Target Cells:
- Kidney tubules (collecting ducts and distal tubules): Primary target.
- Arterioles: Smooth muscle cells.
- Major Functions:
- Increases H₂O Reabsorption: ADH increases the permeability of the collecting ducts and distal tubules to water, leading to increased water reabsorption from the filtrate back into the blood. This concentrates the urine and conserves body water. It achieves this by inserting aquaporin-2 water channels into the luminal membrane of these cells.
- Produces Vasoconstriction: At high concentrations, ADH can cause generalized constriction of arterioles, leading to an increase in total peripheral resistance and arterial blood pressure. This pressor effect is particularly important in cases of severe hemorrhage.
2. Oxytocin
- Synthesis Site: Primarily paraventricular nucleus of the hypothalamus.
- Target Cells:
- Uterus: Smooth muscle cells.
- Mammary Glands (Breasts): Myoepithelial cells surrounding milk-producing alveoli.
- Major Functions:
- Increases Contractility (Uterus): Stimulates uterine smooth muscle contraction, particularly important during childbirth (positive feedback loop during labor).
- Causes Milk Ejection (Let-down Reflex): Stimulates the contraction of myoepithelial cells in the mammary glands, forcing milk from the alveoli into the ducts, making it available for suckling. This is a neuroendocrine reflex triggered by suckling.
C. Anterior Pituitary (Adenohypophysis)
The anterior pituitary synthesizes and secretes six major peptide hormones, often under the control of hypothalamic releasing and inhibiting hormones. Many of these are tropic hormones, regulating other endocrine glands.
1. Thyroid-Stimulating Hormone (TSH, Thyrotropin)
- Target Cells: Thyroid follicular cells.
- Major Functions:
- Stimulates T₃ and T₄ Secretion: TSH binds to receptors on thyroid follicular cells, stimulating all steps of thyroid hormone synthesis and release (iodide trapping, oxidation, organification, coupling, endocytosis, proteolysis, and release of T₃ and T₄).
- Maintains Thyroid Gland Size: TSH has a trophic effect on the thyroid gland, maintaining its growth and vascularity.
2. Adrenocorticotropic Hormone (ACTH, Corticotropin)
- Target Cells: Primarily the zona fasciculata and zona reticularis of the adrenal cortex.
- Major Functions:
- Stimulates Cortisol Secretion: ACTH stimulates these layers of the adrenal cortex to synthesize and secrete glucocorticoids (e.g., cortisol) and adrenal androgens.
- Maintains Adrenal Cortex Integrity: It also has a trophic effect on these layers, maintaining their size and function.
3. Growth Hormone (GH, Somatotropin)
- Target Cells:
- Directly: Bone and soft tissues (skeletal muscle, adipose tissue).
- Indirectly (via IGF-I): Liver (primarily produces IGF-I), bone and soft tissues.
- Major Functions:
- Promotes Overall Growth: GH is essential for normal physical growth throughout childhood and adolescence. Many of its growth-promoting effects are mediated indirectly by stimulating the liver (and other tissues) to produce Insulin-like Growth Factor-I (IGF-I). IGF-I then acts on target cells to promote protein anabolism (increased amino acid uptake and protein synthesis), cell proliferation, and tissue growth, particularly in bone (epiphyseal plate growth) and soft tissues.
- Direct Metabolic Effects: GH also has direct metabolic effects that include:
- Mobilizing fat stores: Increases lipolysis in adipose tissue, leading to increased fatty acid use for energy.
- Conserving glucose: Decreases glucose uptake by tissues and increases glucose output by the liver, thus increasing blood glucose levels (diabetogenic effect).
4. Follicle-Stimulating Hormone (FSH)
- Target Cells (Females): Ovarian follicles.
- Major Functions (Females):
- Promotes Follicular Growth and Development: Stimulates the growth of ovarian follicles in the ovary.
- Stimulates Estrogen Secretion: Acts on granulosa cells within the follicles to promote estrogen synthesis and secretion.
- Target Cells (Males): Seminiferous tubules in testes (specifically Sertoli cells).
- Major Functions (Males):
- Stimulates Sperm Production (Spermatogenesis): Essential for supporting the development of sperm.
5. Luteinizing Hormone (LH)
- Target Cells (Females): Ovarian follicle and corpus luteum.
- Major Functions (Females):
- Stimulates Ovulation: Triggers the rupture of the mature follicle and the release of the egg.
- Corpus Luteum Development: Promotes the formation of the corpus luteum from the ruptured follicle.
- Estrogen and Progesterone Secretion: Stimulates the corpus luteum to secrete progesterone and estrogen after ovulation.
- Target Cells (Males): Interstitial cells of Leydig in testes.
- Major Functions (Males):
- Stimulates Testosterone Secretion: Acts on Leydig cells to promote the synthesis and secretion of testosterone.
6. Prolactin (PRL)
- Target Cells (Females): Mammary glands.
- Major Functions (Females):
- Promotes Breast Development: Contributes to the development of glandular tissue in the breasts during puberty and pregnancy.
- Stimulates Milk Secretion (Lactogenesis): Initiates and maintains milk production after childbirth.
- Target Cells (Males): Unclear, but may play a role in testicular function.
- Major Functions (Males): Uncertain, but high levels can inhibit GnRH secretion, leading to reduced testosterone and infertility.
D. Pineal Gland
The pineal gland is a small endocrine gland located deep in the brain. Its primary hormone is melatonin, which plays a role in regulating circadian rhythms.
- Melatonin
- Target Cells: Brain (anterior pituitary, suprachiasmatic nucleus), reproductive organs, immune system, and possibly others.
- Major Functions:
- Entrains Body's Biological Rhythm (Circadian Rhythm): Melatonin secretion is high during darkness and low during light, providing the body with a "darkness signal." This helps synchronize the body's internal clock (circadian rhythm) with the external light-dark cycle, influencing sleep-wake cycles.
- Inhibits Gonadotropins: Its reduction (as light exposure increases with age) is thought to be involved in the initiation of puberty. High melatonin levels in childhood may inhibit the release of GnRH.
- Antioxidant & Immune Enhancement: Functions as a potent antioxidant, protecting cells from oxidative stress. It also influences immune function.
II. Peripheral Endocrine Glands
These glands are distributed throughout the body and have diverse, specialized functions.
A. Thyroid Gland
Located in the neck, the thyroid gland produces thyroid hormones that regulate metabolism and calcitonin that influences calcium balance.
- Tetraiodothyronine (T₄, Thyroxine) & Triiodothyronine (T₃)
- Synthesized by: Thyroid follicular cells.
- Target Cells: Most cells in the body.
- Major Functions:
- Increases Metabolic Rate: Increases oxygen consumption and heat production, boosting the basal metabolic rate. This affects the metabolism of carbohydrates, fats, and proteins.
- Essential for Normal Growth and Nerve Development: Critical for proper nervous system development in children and for maintaining normal neurological function in adults. It also plays a permissive role in the actions of Growth Hormone.
- Calcitonin
- Synthesized by: Thyroid C cells (parafollicular cells).
- Target Cells: Bone (osteoclasts primarily).
- Major Functions:
- Decreases Plasma Ca²⁺ Concentration: When blood calcium levels are high, calcitonin is released. It inhibits osteoclast activity (which break down bone and release calcium) and stimulates osteoblast activity (which build bone and store calcium), thereby promoting calcium deposition into bone and lowering blood calcium levels. Its physiological role in humans is generally considered less significant than PTH in normal calcium homeostasis.
B. Adrenal Glands
Two glands located atop the kidneys, each composed of an outer cortex and an inner medulla, producing different sets of hormones.
1. Adrenal Cortex
The outer part of the adrenal gland, divided into three zones, each producing distinct steroid hormones.
Zona Glomerulosa
- Hormone: Aldosterone (a mineralocorticoid).
- Target Cells: Kidney tubules (distal and collecting tubules).
- Major Functions:
- Increases Na⁺ Reabsorption: Stimulates the reabsorption of sodium ions from the kidney tubules into the blood.
- Increases K⁺ Secretion: Promotes the secretion of potassium ions from the blood into the kidney tubules for excretion. These actions contribute to maintaining blood volume, blood pressure, and electrolyte balance.
Zona Fasciculata and Zona Reticularis
- Hormone: Cortisol (a glucocorticoid).
- Target Cells: Most cells in the body.
- Major Functions:
- Increases Blood Glucose: Increases blood glucose levels by promoting gluconeogenesis (glucose formation from non-carbohydrate sources) in the liver and reducing glucose uptake by peripheral tissues (at the expense of protein and fat stores).
- Contributes to Stress Adaptation: Plays a critical role in the body's response to stress by mobilizing energy stores and suppressing immune and inflammatory responses.
- Immunosuppressive and Anti-inflammatory: Pharmacological doses are used to suppress the immune system and reduce inflammation.
- Hormone: Androgens (Dehydroepiandrosterone, DHEA).
- Target Cells: Primarily bone and brain (in females, other tissues convert DHEA into more potent androgens or estrogens).
- Major Functions:
- Pubertal Growth Spurt and Sex Drive: In females, adrenal androgens contribute to the pubertal growth spurt and are the primary source of sex drive (libido). In males, their role is less significant compared to testicular androgens.
2. Adrenal Medulla
The inner part of the adrenal gland, derived from neural tissue, secreting catecholamines.
- Hormones: Epinephrine (Adrenaline) and Norepinephrine (Noradrenaline) (catecholamines).
- Target Cells: Sympathetic receptor sites throughout the body (adrenergic receptors on various organs and tissues).
- Major Functions:
- Reinforce Sympathetic Nervous System: Act as hormones to augment and prolong the effects of sympathetic nervous system activation, preparing the body for "fight or flight."
- Contribute to Stress Adaptation: Mobilize energy stores (increase glucose and fatty acids in blood), increase heart rate and contractility, vasoconstrict/vasodilate specific blood vessels to redistribute blood flow, and dilate airways.
- Blood Pressure Regulation: Contribute to the acute regulation of blood pressure.
C. Endocrine Pancreas (Islets of Langerhans)
Clusters of endocrine cells within the pancreas that regulate blood glucose levels.
1. Insulin (from β cells)
- Target Cells: Most cells in the body (especially skeletal muscle, adipose tissue, and liver).
- Major Functions:
- Promotes Cellular Uptake, Use, and Storage of Absorbed Nutrients: Primarily lowers blood glucose by:
- Increasing glucose uptake by insulin-sensitive cells (muscle, adipose tissue) through the insertion of GLUT4 transporters.
- Promoting glycogenesis (glucose to glycogen) in liver and muscle.
- Promoting fat synthesis (lipogenesis) and inhibiting lipolysis in adipose tissue.
- Promoting protein synthesis.
- Overall Anabolic Hormone: Dominant during the absorptive (fed) state.
- Promotes Cellular Uptake, Use, and Storage of Absorbed Nutrients: Primarily lowers blood glucose by:
2. Glucagon (from α cells)
- Target Cells: Most cells in the body (primarily liver, but also adipose tissue).
- Major Functions:
- Maintains Nutrient Levels in Blood During the Postabsorptive State: Primarily raises blood glucose by:
- Promoting glycogenolysis (glycogen breakdown to glucose) in the liver.
- Promoting gluconeogenesis in the liver.
- Increasing lipolysis in adipose tissue to provide fatty acids for energy and glycerol for gluconeogenesis.
- Overall Catabolic Hormone: Dominant during the post-absorptive (fasting) state.
- Maintains Nutrient Levels in Blood During the Postabsorptive State: Primarily raises blood glucose by:
3. Somatostatin (from δ cells)
- Target Cells: Digestive system (pancreatic α and β cells, GI tract cells).
- Major Functions:
- Inhibits Digestion and Absorption of Nutrients: Acts as a local paracrine to inhibit the secretion of insulin and glucagon from the pancreas.
- It also suppresses the motility and secretion of the GI tract, slowing down the rate of nutrient absorption.
D. Parathyroid Gland
Typically four small glands located on the posterior surface of the thyroid gland, crucial for calcium homeostasis.
- Parathyroid Hormone (PTH)
- Target Cells: Bone, kidneys, and intestine (indirectly via vitamin D activation).
- Major Functions:
- Increases Plasma Ca²⁺ Concentration: This is its primary role. It achieves this by:
- Bone: Stimulating osteoclast activity, leading to bone resorption and release of calcium (and phosphate) into the blood.
- Kidneys: Increasing renal reabsorption of calcium (reducing urinary calcium excretion) and inhibiting renal reabsorption of phosphate (increasing urinary phosphate excretion).
- Intestine: Stimulating the kidneys to convert vitamin D into its active form (calcitriol), which then increases intestinal absorption of calcium.
- Decreases Plasma PO₄²⁻ Concentration: By increasing phosphate excretion by the kidneys.
- Increases Plasma Ca²⁺ Concentration: This is its primary role. It achieves this by:
E. Female Gonads (Ovaries)
Paired reproductive organs in females, producing female sex hormones.
- Estrogen (e.g., Estradiol)
- Target Cells: Female sex organs and body as a whole.
- Major Functions:
- Promotes Follicular Development: Essential for the growth and maturation of ovarian follicles.
- Governs Development of Female Secondary Sexual Characteristics: Responsible for breast development, widening of hips, and characteristic fat distribution.
- Stimulates Uterine and Breast Growth: Promotes endometrial proliferation in the uterus and breast glandular tissue development.
- Progesterone
- Target Cells: Bone, Uterus.
- Major Functions:
- Prepares for Pregnancy: Induces secretory changes in the endometrium of the uterus to prepare it for implantation and supports pregnancy.
- Promotes Closure of Epiphyseal Plate: Contributes to the cessation of linear bone growth during puberty.
- Inhibin
- Target Cells: Anterior pituitary.
- Major Functions:
- Inhibits Secretion of FSH: Provides negative feedback to the anterior pituitary, helping to regulate FSH levels.
F. Male Gonads (Testes)
Paired reproductive organs in males, producing male sex hormones.
- Testosterone
- Target Cells: Male sex organs and body as a whole.
- Major Functions:
- Stimulates Sperm Production (Spermatogenesis): Essential for the maturation of sperm.
- Governs Development of Male Secondary Sexual Characteristics: Responsible for features like facial hair growth, deepening of voice, and increased muscle mass.
- Promotes Sex Drive (Libido): Influences sexual desire.
- Target Cells: Bone.
- Major Functions:
- Enhances Pubertal Growth Spurt; Promotes Closure of the Epiphyseal Plate: Contributes to rapid growth during puberty and eventually stops linear bone growth.
- Inhibin
- Target Cells: Anterior pituitary.
- Major Functions:
- Inhibits Secretion of FSH: Provides negative feedback to the anterior pituitary, helping to regulate FSH levels.
G. Placenta (during pregnancy)
A temporary organ that connects the mother to the developing fetus, also acting as an endocrine gland.
- Estrogen (e.g., Estriol) and Progesterone
- Target Cells: Female sex organs (uterus, breasts).
- Major Functions:
- Help Maintain Pregnancy: Essential for maintaining the uterine lining and preventing premature contractions.
- Prepare Breasts for Lactation: Contribute to mammary gland development for milk production.
- Human Chorionic Gonadotropin (hCG)
- Target Cells: Ovarian corpus luteum.
- Major Functions:
- Maintains Corpus Luteum of Pregnancy: Prevents the degeneration of the corpus luteum, ensuring continued progesterone (and estrogen) production in early pregnancy until the placenta can take over hormone synthesis. This is the hormone detected in pregnancy tests.
III. Organs With Secondary Endocrine Functions
Many organs primarily known for non-endocrine roles also produce and secrete hormones that have significant systemic effects.
A. Kidneys
Beyond their role in filtration and waste excretion, the kidneys produce hormones vital for blood pressure and red blood cell production.
- Renin (by activating angiotensinogen)
- Produced by: Juxtaglomerular cells.
- Target Cells: Acts on angiotensinogen (a plasma protein from the liver) to produce angiotensin I, which is then converted to angiotensin II. Angiotensin II then targets the zona glomerulosa of the adrenal cortex.
- Major Functions:
- Stimulates Aldosterone Secretion: Angiotensin II is a powerful stimulus for aldosterone release from the adrenal cortex.
- Potent Vasoconstrictor: Angiotensin II directly constricts blood vessels throughout the body, increasing total peripheral resistance and blood pressure.
- Stimulates Thirst: Contributes to fluid intake regulation.
- (Part of the Renin-Angiotensin-Aldosterone System - RAAS, which regulates blood pressure and fluid balance).
- Erythropoietin
- Produced by: Peritubular cells in the renal cortex.
- Target Cells: Bone marrow (specifically erythrocyte progenitor cells).
- Major Functions:
- Stimulates Erythrocyte Production: Acts on the bone marrow to stimulate the proliferation and differentiation of red blood cell precursors, leading to increased red blood cell mass. This is a crucial response to hypoxia.
B. Stomach
The stomach is involved in digestion but also produces hormones that regulate appetite and digestive processes.
- Ghrelin
- Produced by: P/D1 cells in the fundus of the stomach.
- Target Cells: Hypothalamus (arcuate nucleus).
- Major Functions:
- Signals Hunger, Stimulates Appetite: Often called the "hunger hormone," its levels rise before meals and fall after, signaling the brain to initiate food intake.
- Gastrin
- Produced by: G cells in the pyloric antrum.
- Target Cells: Digestive tract exocrine glands (e.g., parietal cells, chief cells) and smooth muscles of the stomach, pancreas, liver, gallbladder.
- Major Functions:
- Controls Motility and Secretion: Primarily stimulates the secretion of gastric acid (HCl) by parietal cells and promotes gastric motility, facilitating digestion and absorptive processes. It also has trophic effects on the gastric mucosa.
C. Small Intestine
The small intestine produces several hormones that coordinate digestion and nutrient absorption.
- Secretin and Cholecystokinin (CCK)
- Secretin produced by: S cells in the duodenum.
- CCK produced by: I cells in the duodenum and jejunum.
- Target Cells: Primarily endocrine pancreas (for insulin secretion), but also exocrine pancreas, gallbladder, stomach.
- Major Functions:
- Stimulates Insulin Secretion: While their primary roles are related to exocrine secretions (e.g., secretin stimulates bicarbonate-rich fluid from the pancreas; CCK stimulates enzyme-rich fluid from the pancreas and gallbladder contraction), they also have an "incretin effect" indirectly stimulating insulin secretion in response to nutrient presence.
- Glucose-Dependent Insulinotropic Peptide (GIP, Gastric Inhibitory Peptide)
- Produced by: K cells in the duodenum and jejunum.
- Target Cells: Endocrine pancreas (β cells).
- Major Functions:
- Stimulates Insulin Secretion: A major incretin hormone, GIP significantly enhances insulin release from pancreatic β-cells in response to oral glucose intake, anticipating the rise in blood glucose.
- Peptide YY₃-₃₆ (PYY)
- Produced by: L cells in the ileum and colon.
- Target Cells: Hypothalamus (arcuate nucleus).
- Major Functions:
- Signals Satiety, Suppresses Appetite: Released post-prandially, PYY helps to signal fullness and reduce food intake, contributing to short-term satiety.
D. Liver
The liver is a metabolic powerhouse and also an endocrine organ.
- Insulin-like Growth Factor-I (IGF-I, Somatomedin C)
- Produced by: Liver (primarily) in response to Growth Hormone.
- Target Cells: Bone and soft tissues.
- Major Functions:
- Promotes Growth: Mediates many of the growth-promoting effects of Growth Hormone, stimulating cell proliferation, protein synthesis, and linear growth, particularly in cartilage and bone.
- Thrombopoietin
- Produced by: Liver (primary site) and kidneys.
- Target Cells: Bone marrow (megakaryocytes).
- Major Functions:
- Stimulates Platelet Production: Regulates the production of platelets by stimulating the growth and differentiation of megakaryocytes in the bone marrow.
- Hepcidin
- Produced by: Liver.
- Target Cells: Intestine (duodenal enterocytes), macrophages.
- Major Functions:
- Inhibits Iron Absorption into Blood: The master regulator of iron homeostasis. It controls the release of iron from enterocytes, macrophages, and hepatocytes into the plasma, thereby reducing intestinal iron absorption and preventing iron overload.
E. Skin
The skin plays a crucial role in vitamin D synthesis, a hormone precursor.
- Vitamin D (active form, Calcitriol)
- Precursor produced in: Skin (via UV light exposure from 7-dehydrocholesterol). Activated in liver and kidneys.
- Target Cells: Intestine (enterocytes), bone, kidneys.
- Major Functions:
- Increases Absorption of Ingested Ca²⁺ and PO₄²⁻: The active form of vitamin D (1,25-dihydroxyvitamin D₃ or calcitriol) acts as a hormone, primarily stimulating the intestinal absorption of calcium and phosphate, contributing to bone mineralization and maintaining plasma calcium levels.
F. Thymus
A lymphatic organ located in the chest, primarily active in childhood and crucial for immune system development.
- Thymosin
- Produced by: Thymus.
- Target Cells: T lymphocytes (thymocytes).
- Major Functions:
- Enhances T Lymphocyte Proliferation and Function: Involved in the maturation and differentiation of T lymphocytes, essential for cell-mediated immunity.
G. Heart
The heart, primarily a circulatory organ, also produces hormones involved in fluid and electrolyte balance.
- Atrial and Brain Natriuretic Peptides (ANP, BNP)
- ANP produced by: Atrial muscle cells (primarily).
- BNP produced by: Ventricular muscle cells (primarily).
- Target Cells: Kidney tubules, adrenal cortex, blood vessels.
- Major Functions:
- Inhibit Na⁺ Reabsorption: Promote the excretion of sodium and water by the kidneys (natriuresis and diuresis), thereby reducing blood volume and blood pressure.
- Vasodilation: Cause vasodilation, further lowering blood pressure.
- Inhibit Renin and Aldosterone Secretion: Suppress the RAAS.
H. Adipose Tissue
Far from being just a storage depot, adipose tissue is an active endocrine organ.
- Leptin
- Produced by: Adipocytes (fat cells).
- Target Cells: Hypothalamus (arcuate nucleus).
- Major Functions:
- Suppresses Appetite, Important in Long-Term Control of Body Weight: Signals satiety to the brain, informing it about the body's energy stores. Higher leptin levels (indicating more fat) typically lead to decreased appetite and increased energy expenditure.
- Other Adipokines (e.g., Adiponectin, Resistin, inflammatory cytokines)
- Produced by: Adipocytes.
- Target Cells: Multiple sites (liver, muscle, immune cells).
- Major Functions:
- Play a Role in Metabolism and Inflammation: These hormones influence insulin sensitivity, glucose and lipid metabolism, and immune responses, linking obesity to metabolic disorders and chronic inflammation.
Classification of hormones depending upon chemical nature
| Steroids | Proteins | Derivatives of tyrosine |
|---|---|---|
|
Aldosterone 11-deoxycorticosterone Cortisol Corticosterone Testosterone Dihydrotestosterone Dehydroepiandrosterone Androstenedione Estrogen Progesterone |
Growth hormone (GH) Thyroid-stimulating hormone (TSH) Adrenocorticotropic hormone (ACTH) Follicle-stimulating hormone (FSH) Luteinizing hormone (LH) Prolactin Antidiuretic hormone (ADH) Oxytocin Parathormone Calcitonin Insulin Glucagon Somatostatin Pancreatic polypeptide Human chorionic gonadotropin (HCG) Human chorionic somatomammotropin. |
Thyroxine (T₄) Triiodothyronine (T₃) Adrenaline (Epinephrine) Noradrenaline (Norepinephrine) Dopamine. |